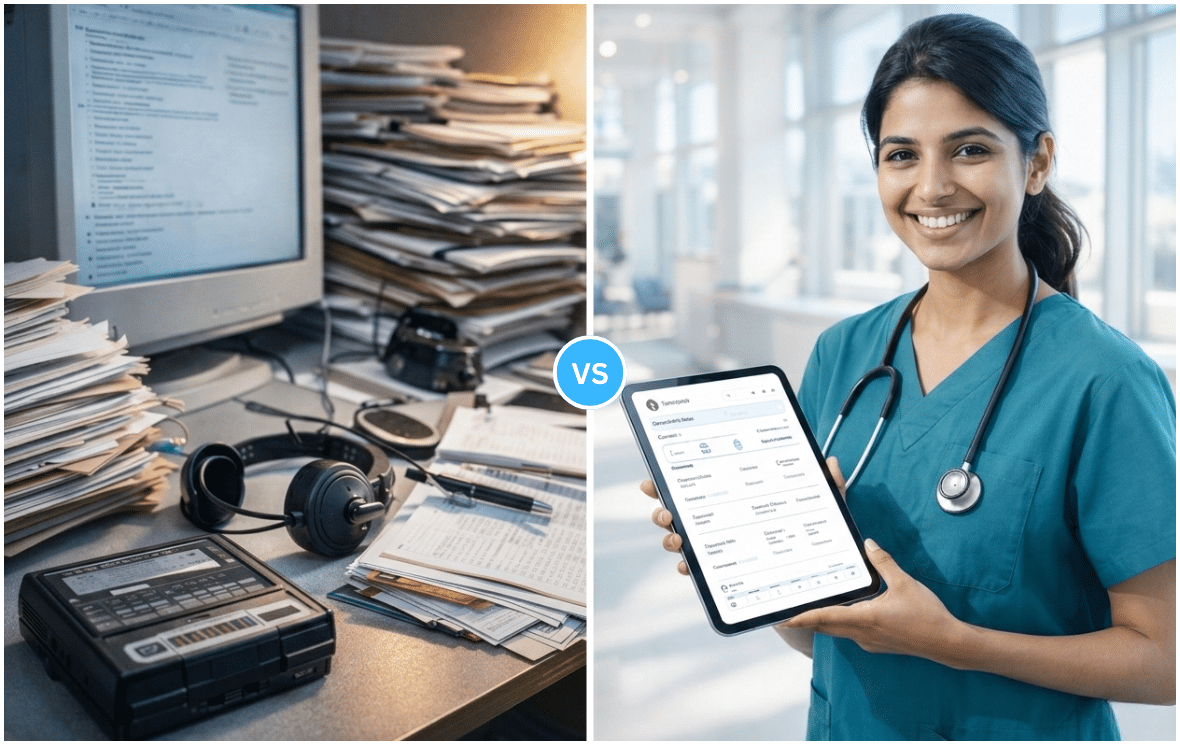
Clinical documentation has become one of the biggest operational pressures in modern healthcare. In 2026, documentation is no longer just about keeping records, it directly affects physician burnout, reimbursement timelines, compliance risk, and patient satisfaction.
Studies consistently show that physicians spend 15–20 hours per week on documentation-related work, and for every 1 hour of patient interaction, nearly 2 additional hours are spent on EHR and administrative tasks. After-hours charting, often called “pajama time” – remains a leading contributor to burnout across ambulatory practices.
For decades, traditional medical transcription helped reduce typing workload by converting dictations into structured notes, often supported by dedicated medical transcription software platforms.
This model improved efficiency compared to manual entry but introduced:
- 24–72 hour turnaround times
- Per-line or per-minute pricing structures
- Manual EHR uploads
- Revision cycles that delay billing
In contrast, AI medical scribe software uses ambient listening and clinical AI models to generate structured notes in real time. Instead of dictating after a visit, providers receive near-instant documentation during or immediately after the encounter.
The shift toward AI medical scribe vs traditional medical transcription is accelerating, as more practices compare traditional medical transcription vs AI solutions for long-term efficiency.
- Same-day chart completion
- Faster billing submission
- Reduced administrative burden
- Scalable documentation workflows
- Predictable SaaS-based pricing
Industry adoption trends in 2026 show a steady migration away from purely human transcription models toward AI-assisted clinical documentation tools, especially in outpatient and specialty clinics.
Choosing between medical transcription vs AI documentation is no longer a minor workflow preference. It impacts:
- Cost per patient encounter
- Revenue cycle efficiency
- Compliance risk exposure
- Provider retention
- Long-term scalability
When documentation delays impact AI in healthcare billing efficiency.
This guide provides a data-driven comparison to help healthcare leaders make an informed, future-ready decision.
Curious how real-time AI documentation works in practice?
👉 Book a live demo to see structured clinical notes generated instantly within your EHR.
What Is Traditional Medical Transcription?
Traditional medical transcription is a documentation process where physicians record patient encounter notes via dictation, and a trained transcriptionist converts the audio into structured medical records.
Although this model has supported healthcare for decades, its workflow was designed for a pre real-time era, before AI clinical documentation tools and ambient scribing became widely available.
Traditional Transcription: Key Categories
| Categories | Traditional Medical Transcription |
| Documentation Method | Dictation + human transcriptionist |
| Turnaround Time | 24–72 hours |
| Pricing Model | Per line / per minute |
| EHR Integration | Manual upload or copy-paste |
| Accuracy | Dependent on human skill & audio clarity |
| Revisions | Common if audio unclear |
| Scalability | Cost increases with volume |
| After-Hours Work | Physicians often dictate after clinic hours |
Pros of Using Traditional Medical Transcription
- Familiar Dictation Workflow : Many physicians are already comfortable dictating notes, reducing the need for retraining or workflow disruption.
- Human Review & Context Recognition : Experienced transcriptionists can sometimes interpret nuanced speech patterns, accents, or specialty-specific terminology.
- No Real-Time Technology Dependency : Does not require ambient listening software or advanced AI tools during the patient visit.
- Flexible Outsourcing Options : Practices can outsource transcription services without investing in in-house documentation infrastructure.
- Minimal Software Learning Curve : Providers who prefer voice recording over structured templates may find it easier to adopt.
Cons of Using Traditional Medical Transcription
- Delayed Turnaround Time (24–72 Hours) : Notes are not immediately available, potentially delaying billing and care coordination.
- Variable & Increasing Costs : Per-line or per-minute pricing models scale with patient volume, increasing operational expenses over time.
- Manual EHR Integration : Notes often require manual review, formatting, or upload into the EHR system.
- Revision Cycles Can Slow Documentation : Unclear dictation may require clarification, causing additional delays.
- Limited Workflow Automation : Unlike AI medical scribe software, transcription does not provide structured templates, coding suggestions, or real-time documentation assistance.
- Workforce Dependency & Outsourcing Risks : Reliance on human transcriptionists may introduce availability constraints or compliance considerations.
Where Traditional Transcription Still Makes Sense
Traditional medical transcription may still be appropriate in specific scenarios:
- Low-Volume Solo Practices
Providers seeing fewer patients daily may not experience significant workflow pressure. - Clinics with Limited Technology Infrastructure
Rural or bandwidth-limited settings may prefer offline dictation models. - Physicians Highly Comfortable with Dictation
Some providers prefer reviewing transcribed notes rather than relying on AI-generated documentation. - Practices in Transition Phase
Clinics evaluating AI medical scribe vs traditional medical transcription may temporarily use transcription before fully migrating to AI documentation systems. - Specialty Cases Requiring Detailed Narrative Reports
Certain subspecialties that rely heavily on long-form narrative documentation may still utilize transcription workflows.
What Is an AI Medical Scribe?
An AI medical scribe is a clinical documentation tool that uses artificial intelligence, speech recognition, and natural language processing (NLP) to automatically generate structured medical notes from patient–provider conversations, in real time.
Unlike traditional medical transcription, which converts dictated audio after the visit, AI medical scribe software listens during the encounter (ambient documentation) and produces structured notes instantly or within minutes.
Pros of Using AI Medical Scribes (2026)
- Real-Time Documentation : Generates structured clinical notes during or immediately after the patient encounter, reducing chart completion delays.
- Significant Time Savings : Helps reduce documentation workload, allowing physicians to spend more time with patients instead of the EHR.
- Reduced After-Hours Charting (“Pajama Time”) : Many practices report improved same-day note completion, lowering burnout risk.
- Predictable Subscription Pricing : Monthly SaaS models replace per-line variable transcription costs, improving budgeting accuracy.
- Direct EHR Integration : AI medical scribe software typically syncs notes directly into the EHR, minimizing manual uploads through secure EHR integration frameworks.
- Structured & Standardized Notes : Automatically formats SOAP notes, specialty templates, and structured fields for consistency.
- AI Progress Generator : Many practices now rely on an AI progress note generator to automatically structure SOAP notes and specialty templates within seconds.
- Scalable for Growing Practices : Supports multi-provider and multi-location clinics without proportional cost increases.
- Workflow Automation Beyond Transcription : Some AI documentation tools assist with coding support, template optimization, and structured data capture.
Unlike automated medical transcription software that only converts speech to text, AI scribes generate structured and clinically relevant notes.
Cons of Using AI Medical Scribes
- Initial Adoption Curve : Providers may need short onboarding time to adjust to ambient documentation workflows.
- Technology Dependence : Requires stable internet and EHR compatibility.
- Speech Recognition Limitations : Accuracy can vary depending on accents, specialty complexity, or background noise.
- Compliance Evaluation Required : Practices must ensure the AI medical scribe vendor meets HIPAA and data security standards, including encrypted storage and HIPAA-compliant AI documentation protocols.
- Subscription Cost Consideration : Monthly pricing may feel higher upfront compared to low-volume transcription usage.
AI Medical Scribe vs Traditional Transcription (Core Difference)
| Core Function | Traditional Transcription | AI Medical Scribe |
| Converts Speech to Text | ✅ Yes | ✅ Yes |
| Understands Clinical Context | ❌ Limited | ✅ Advanced NLP |
| Generates Structured SOAP Notes | ❌ Manual formatting | ✅ Automatic |
| Works During Patient Visit | ❌ No | ✅ Yes |
| Real-Time Documentation | ❌ No | ✅ Yes |
| Automation Beyond Typing | ❌ No | ✅ Yes |
How AI Medical Scribe Technology Works
AI medical scribes combine multiple technologies, including advanced medical speech to text software capabilities:
1. Ambient Speech Recognition
The system captures provider–patient conversations during the visit without requiring active dictation.
2. Natural Language Processing (NLP)
Clinical language models identify:
- Symptoms
- Diagnoses
- Medications
- Procedures
- Assessment & plan components
3. Clinical Context Understanding
Advanced AI documentation tools distinguish between:
- Patient statements
- Provider observations
- Clinical decision-making elements
4. Structured Note Generation
The system formats documentation into:
- SOAP notes
- Specialty templates
- Problem-based charting
- Structured EHR fields
| Step | AI Medical Scribe Process |
| 1 | Provider begins patient encounter |
| 2 | AI passively captures conversation |
| 3 | AI processes context in real time |
| 4 | Structured note is generated |
| 5 | Provider reviews and signs off |
| 6 | Note syncs directly into EHR |
This AI charting solution ensures consistent documentation formatting across providers and specialties, especially when integrated into modern clinical notes software systems.
Want to see this workflow in action?
👉 Explore Murphi’s AI medical scribe and how it integrates directly with your clinical documentation process.
Who Should Choose Traditional Transcription?
While AI medical scribe software is growing rapidly, traditional medical transcription may still be appropriate in certain scenarios:
- Solo or Low-Volume Providers : Practices seeing fewer patients per day may not experience enough documentation pressure to justify full AI automation.
- Providers Comfortable with Dictation Workflows : Physicians who prefer recording notes after visits and reviewing formatted transcripts may find this workflow familiar and reliable.
- Clinics with Limited Technology Infrastructure : Settings with unstable internet connectivity or limited EHR integration capability may rely on transcription services.
- Transitional Practices : Clinics evaluating AI medical scribe vs traditional medical transcription may temporarily continue transcription while assessing AI documentation tools.
- Narrative-Heavy Specialties : Some subspecialties that rely on long-form descriptive reporting may still prefer human-formatted documentation.
Who Should Choose AI Medical Scribes in 2026?
In 2026, AI medical scribes are increasingly suited for growth-oriented and efficiency-focused practices.
- High-Volume Outpatient Clinics : Real-time documentation supports faster patient turnover and same-day chart completion.
- Multi-Provider or Multi-Location Practices : Enterprise organizations may also explore a white-label AI medical scribe platform to standardize documentation across locations.
- Burnout-Conscious Organizations : Reducing after-hours charting helps improve provider satisfaction and retention.
- Practices Focused on Revenue Cycle Optimization : Faster documentation leads to earlier claim submission and improved cash flow, directly strengthening your revenue cycle management performance.
- Value-Based Care & Quality Reporting Models : Structured AI-generated notes help support standardized documentation and data capture.
- Clinics Seeking Long-Term Operational Efficiency : AI medical scribes function as documentation automation systems, not just transcription tools, often powered by specialized AI agents for healthcare.
An AI scribe for doctors can significantly reduce after-hours documentation and administrative fatigue.
FAQs For AI Medical Scribe vs Traditional Medical Transcription
- Is AI medical scribe better than transcription?
AI medical scribes provide real-time structured documentation and reduce after-hours charting. Traditional transcription converts dictated audio to text but usually involves delays. The better option depends on workflow goals and scalability needs.
- Are AI scribes HIPAA compliant?
Most reputable AI medical scribe vendors design their platforms to meet HIPAA security standards. Practices should verify data encryption, access controls, and audit logging before implementation.
- How accurate are AI medical scribes?
Modern AI medical scribes use advanced clinical language models and can achieve high contextual accuracy. However, Physician review and sign-off remain essential to reduce documentation risk and medical errors.
- Do AI scribes replace medical transcriptionists?
AI scribes automate much of the documentation process. While they reduce reliance on traditional transcription, human oversight and quality review roles may still exist.
- How much does an AI medical scribe cost in 2026?
In 2026, AI medical scribe software typically ranges between $400–$900 per provider per month, depending on features and integrations, as outlined in this detailed breakdown of AI medical scribe cost.
- Can AI scribes integrate with EHR systems?
Yes. Most modern AI clinical documentation tools integrate directly with major EHR platforms, enabling automatic note syncing and structured data entry.
- What is the main difference between AI medical scribe and transcription?
Transcription converts dictated speech into text. AI medical scribes generate structured clinical documentation in real time using contextual understanding.
- Is AI documentation secure for patient data?
Security depends on the vendor. Leading AI medical scribe solutions implement encrypted data transmission, access controls, and compliance monitoring.
- How does AI vs human medical transcription accuracy compare?
AI systems provide consistent structured formatting, while human transcription may capture nuanced phrasing. Most practices use physician review to ensure clinical accuracy in both models.
Conclusion
Clinical documentation is no longer just about typing efficiency, it directly influences physician workload, revenue cycle speed, and practice scalability.
Traditional medical transcription remains a viable option for certain low-volume or technology-limited environments. However, its delayed workflow and variable cost structure make it less aligned with the efficiency demands of 2026.
AI medical scribe software represents a shift from documentation support to full-scale automation in healthcare. With real-time note generation, scalable pricing, and workflow integration, it is increasingly becoming the preferred model for growth-focused practices.
Healthcare documentation automation is becoming a strategic priority for modern medical practices adopting AI for clinical workflows.
Clear Recommendation for 2026
Practices aiming to reduce documentation burden, improve billing timelines, and enhance operational efficiency are increasingly choosing AI medical scribes over traditional transcription models.
Final Thought
Clinics looking to reduce documentation time and improve operational efficiency are increasingly adopting AI medical scribes over traditional transcription.
If your organization is evaluating AI medical scribe vs traditional medical transcription, the key question is not just cost, it’s which system supports your long-term growth, compliance, and provider satisfaction goals.